|
 |
- Search
| Ann Child Neurol > Volume 31(3); 2023 > Article |
|
Abstract
Purpose
The aim of this study was to compare sleep problems between children with transfusion-dependent hemoglobinopathies and healthy controls.
Methods
This study was a case-control survey of children with transfusion-dependent hemoglobinopathies. The sample consisted of 175 children in the patient group and 175 healthy children in the control group, with an age range of 8 to 18 years. Subjects were recruited from the Children's Hospital of Mansoura University between February and July 2022. Children with transfusion-dependent hemoglobinopathies received consultations at the Department of Pediatric Hematology. The ChildrenŌĆÖs Sleep Habits Questionnaire (CSHQ) was used to evaluate sleep problems in both groups.
Results
The mean age of the patient group was 11.22┬▒2.39 years, and 52.57% (n=92) were girls. The control group had a mean age of 11.30┬▒2.16 years, and 50.86% (n=89) were boys. The overall score (P=0.007) and the night waking (P=0.013), sleep duration (P=0.009), and sleep-disordered breathing (P=0.029) subscores were all substantially and statistically significantly higher in children with transfusion-dependent hemoglobinopathies than in healthy children.
Hereditary hemoglobin diseases, often known as hemoglobinopathies, are a set of hereditary illnesses involving the structure of hemoglobin. Sickle cell disease (SCD) and thalassemias constitute the majority of these conditions [1,2]. These illnesses are among the most prevalent inherited conditions in the world; the birth rate of individuals who are homozygous or compound heterozygous for symptomatic hemoglobin disorders is around 2.4 per 1,000 births, of whom 1.96 have SCD and 0.44 have thalassemia [3,4].
A ╬▓-globin gene mutation produces sickle hemoglobin, which fills red blood cells and changes their shape and flexibility (the "sickling" process). Exercise and oxidative stress enhance cellular dehydration. Hemoglobin deoxygenation and the intracellular sickle cell hemoglobin concentration affect sickling, polymerization, and severity [5,6]. A vaso-occlusive or hemolytic pathophysiology generates acute and persistent SCD symptoms [7,8]. Vaso-occlusive disease causes chest discomfort and osteonecrosis, while hemolysis causes pulmonary hypertension, priapism, and leg ulcers [9,10]. Thalassemias are hereditary. Hemoglobin develops with two ╬▓-chains and two ╬▒-chains [11,12]. In ╬▒-thalassemia, the ╬▒-globin gene cluster is altered, whereas beta-thalassemia involves mutations in the gene coding for ╬▓-globin. Depending on normal hemoglobin, thalassemia may range from almost asymptomatic to severe anemia needing lifelong blood transfusions and organ damage [13].
Transfusion-dependent hemoglobinopathies cause nocturnal oxyhemoglobin desaturation in 40% of affected children [14]. Oxyhemoglobin levels may drop significantly in children with transfusion-dependent hemoglobinopathies compared to healthy controls, and the severity of SCD is proportional to the extent of desaturation. Daytime hemoglobin saturation is lower in sickle cell anemia patients, lowering their blood oxygen levels. Adenotonsillar hypertrophy-related obstructive sleep apnea (OSA) or SCD-related chronic lung illness may cause hypoxemia [15].
Sleep-disordered breathing occurs when nightly ventilation patterns or amounts are incorrect. OSA, the most common type of sleep-disordered breathing, occurs when the upper airway collapses, reducing airflow and causing hypoxia, sleep disruptions, hypercapnia, and neurocognitive impairment [16]. Snoring, the most common symptom of upper airway resistance, causes sleep-disordered breathing in 7% to 13% of healthy children ages 2 to 8 and 3% to 5% of older children. Sleep-disordered breathing may cause behavioral challenges, learning difficulties, pulmonary hypertension, arterial hypertension, nocturnal enuresis, and developmental concerns in children [17].
Oxygen desaturation below 85% was found to be four times more likely in people with transfusion-dependent hemoglobinopathies and sleep apnea than in people with SCD and no sleep apnea [18]. A spleen injury during childhood may cause enlarged tonsils and adenoids, which may restrict airflow and cause sleep-disordered breathing. These alterations in nocturnal respiration may cause nocturnal hypoxemia due to SCD-enhanced sleep-disordered breathing [19].
Sleep is one of the essential daily requirements for humans. Sleep promotes cellular regeneration, relaxation, comfort, and physical-mental rest. Numerous studies have shown that sleep disturbances are particularly common in sick people [20]. Children with chronic illnesses are affected by a variety of physical and behavioral issues, including sleep disturbances. Chronic illnesses are a leading cause of disability and death. Studies have shown that 30% to 75% of newly diagnosed cancer patients experience a range of sleep difficulties [21]. These patients' sleep disturbances result in chronic weariness, decreased adherence to therapy, and a diminished quality of life [22].
Only 17% of people with a sleep disturbance are checked and treated by doctors, despite the significance of sleep quality [23]. Transfusion-dependent hemoglobinopathies cause various psychological and physical difficulties in sufferers. In particular, these patients often experience a high degree of worry, which disrupts their sleep [24]. However, little research has been undertaken on this topic [25].
Sleep-related disorders are sleep-pattern-altering abnormalities that result in inadequate or poor-quality sleep. Sleep-disordered breathing (e.g., OSA and upper airway obstruction), restless legs syndrome, and insomnia are sleep disorders that make it difficult to begin or sustain high-quality sleep [26]. In the general pediatric population, sleep difficulties are linked with poor effects on learning and attention, diminished cognition, behavioral issues, and reduced health-related quality of life [21].
Considering the high prevalence of snoring and other sleep problems in children with transfusion-dependent hemoglobinopathies and given the time constraints of busy pediatricians to screen for sleep disorders, screening tools have been developed to assist pediatricians in recognizing these symptoms [27]. These questionnaires are comprehensive and are capable of predicting the probability of sleep disorders with a relatively high degree of accuracy [28].
A polysomnographic study (PSG) is the diagnostic technique of choice for quantifying sleep-disordered breathing and sleep architecture. PSG can be performed in children of all ages [29]. PSG is not only useful for diagnosis, but also allows the severity of the disease to be estimated, despite certain limitations: PSG is intrusive, cumbersome, and cost-prohibitive, and facilities that can provide PSG-based diagnostic services in children are not widely available. Furthermore, normative values are based on the statistical distribution of data, and to date, abnormal PSG variables seen in children with OSA have failed to predict adverse clinical outcomes [30].
Given the limitations of PSG, several screening studies have been suggested as a means to distinguish primary snoring and OSA. These studies are based on the frequency and severity of the three cardinal symptoms of sleep apnea: snoring, labored breathing, and oxygen desaturation [31]. Nap studies and overnight oximetry studies have high specificity but low sensitivity; thus, overnight PSG is needed to make the diagnosis in children with negative studies. The other limitations of screening studies include difficulty in estimating the severity of the disease, inability to exclude causes of hypoxemia other than OSA, and an inability to diagnose upper airway resistance syndrome and obstructive hypoventilation, which are other variants of sleep-disordered breathing in children [32].
To the best of our knowledge, existing research on the sleeping patterns and behaviors of children and adolescents with transfusion-dependent hemoglobinopathies, which cause chronic hemolytic anemia, is inadequate [33]. This study intended to compare sleep difficulties between children with transfusion-dependent hemoglobinopathies and healthy controls [34].
The aim of this study was to compare sleep problems between children with transfusion-dependent hemoglobinopathies and healthy controls.
A convenience sample of 175 children with transfusion-dependent hemoglobinopathies who attended the inpatient hematology department and outpatient hematology clinic of the Children's Hospital of Mansoura University was selected for this study, and 175 healthy controls completed the study requirements and were included in the study. In total, 405 children, ranging in age from 8 to 18 years, attended the above-mentioned departments during the 6-month period from February 1, 2021 to July 31, 2022. An assessment for hemoglobinopathy often comprises tests that identify the different forms of hemoglobin and quantify their levels. The information obtained from these tests, in conjunction with the outcomes of standard tests such as a complete blood count, a blood smear, and electrophoresis of globin proteins, helps to reach a diagnosis. There are two categories of children who are diagnosed with hemoglobinopathies: those who need regular blood transfusions (transfusion-dependent) and those who do not (non-transfusion-dependent).
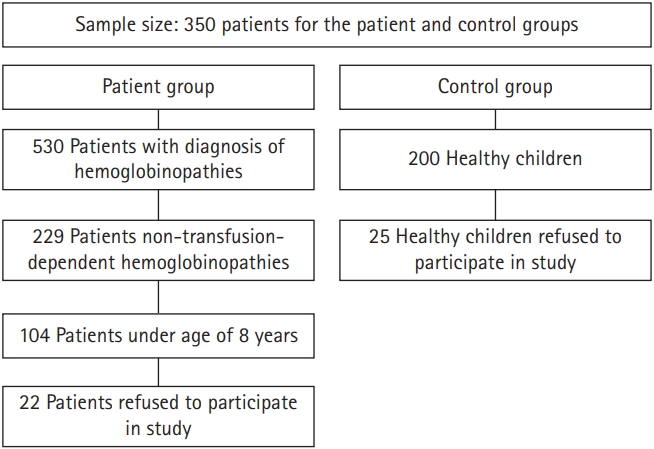
The subjects of this study were required to meet the following criteria (Fig. 1):
ŌĆā(1) Age: between 8 and 18 years
ŌĆā(2) Sex: both sexes
ŌĆā(3) Children who visited the outpatient clinic and inpatient department of the Children's Hospital of Mansoura University.
ŌĆā(4) Children who were blood transfusion-dependent
The exclusion criteria comprised patients with co-morbid illnesses, such as intellectual disability, endocrinological diseases (e.g., diabetes mellitus), cardiovascular diseases, respiratory problems (e.g., asthma), kidney disease (e.g., renal failure), and neurological disorders (e.g., epilepsy and seizures). For context regarding the subjectsŌĆÖ educational level, the public education system in Egypt consists of three levels: the primary educational level for 6 years, starting from 6 to 11 years of age; preparatory school for 3 years, starting from 12 to 14 years of age; and, the secondary school stage for 3 years, from ages 15 to 17 years of age.
Information was collected on childrenŌĆÖs sociodemographic characteristics and clinical data using a sheet designed by the researcher based on a review of the literature for the collection of sociodemographic data from children and their caregivers. The variables included (1) sociodemographic data of children (age, sex, birth order, and level of education) and (2) clinical data from children with hematological disorders, such as the onset of the disease, duration of illness, frequency of blood transfusion, the presence of any other disease (e.g., diabetes mellitus, heart disease [cardiomegaly], and bone deformities [fractures or osteoporosis]), and the presence of thalassemia in the family (including the number of brothers or sisters affected by thalassemia and the familial relationship between parents).
The Children's Sleep Habits Questionnaire (CSHQ) is a 45-item parent survey that has been used in past studies to evaluate how children sleep and determine whether they have any problems [35]. The CSHQ includes items on bedtime resistance (items 1, 3, 4, 5, 6, and 8), sleep onset delay (item 2), sleep duration (items 9, 10, and 11), sleep anxiety (items 5, 7, 8, and 21), night waking (items 16, 24, and 25), sleep-disordered breathing (items 18, 19, and 20), parasomnias (items 12, 13, 14, 15, 17, 22, and 23), and morning waking/daytime sleepiness (items 26, 27, 28, 29, 30, 31, 32, and 33). Items are rated on a 3-point scale: "usually" if the sleep behavior occurs five to seven times per week; "sometimes" for two to four times per week; and "rarely" for zero to one time per week. Items 1, 2, 3 10, 11, and 26 are reverse-coded.
Parents retrospectively complete the CSHQ and are asked to assess the child's sleep habits over the previous week. It generally takes 5 to 15 minutes to fill out the questionnaire. A total of 41 points has been suggested as a cut-off point, with higher scores considered to be clinically significant. The Arabic version used in the present work was developed through a translation and retranslation process by Asaad and Kahla [36].
The collected data were analyzed using SPSS version 26.0 (IBM Corp., Armonk, NY, USA). Demographic variables were presented using descriptive statistics. Categorical variables were compared using the chi-square test. The Kolmogorov-Smirnov and Shapiro-Wilk tests were used to check the normality of data distribution for all continuous variables. Normally distributed parametric variables were compared between groups using the independent-samples t-test. A P value <0.05 was considered to indicate statistical significance.
Verbal informed consent was obtained from all children and their caregivers. All children and their caregivers were informed of their right to refuse or withdraw at any time. The children's privacy was maintained. Ethical committee approval was obtained from the Research Ethics Committee of the Faculty of Nursing, Mansoura University (MFN-IRB No. 2022-02-0113).
Table 1 shows the frequency distribution of the children according to their sociodemographic and clinical characteristics. Approximately two-thirds (62.86%) of the children in the patient group were in the age group of 8 years to less than 12 years, with a mean age of 11.22┬▒2.39 years. Likewise, almost two-thirds (60.57%) of the children in the control group were in the age group of 8 years to less than 12 years, with a mean age of 11.30┬▒2.16 years. In addition, girls represented a higher percentage (52.57%) in the patient group than in the control group (50.86%). Almost half of the children were first children in both the patient group (41.14%) and the control group (44.57%). Approximately two-thirds of the children were at the primary level in both the patient group (62.86%) and control group (66.29%). Statistically significant differences were not found between the two groups in terms of age, sex, educational level, or birth order.
Table 2 shows the distribution of patients according to their clinical data. More than half of the patients (51.43%) had beta-thalassemia major and a similar percentage (53.71%) had a blood transfusion rate of once monthly. The mean age of children when the disease was diagnosed was 7.49┬▒3.06 months, which was also childrenŌĆÖs mean age of children at the time of the first blood transfusion. More than three-quarters of the studied children (77.71%) had a related disease that was detected urgently. Most of the children (80.57%) had splenomegaly, the majority (79.43%) had cardiomegaly, approximately three-quarters of the children (71.43%) had hepatomegaly, over four-fifths of the study children (85.14%) had osteoporosis, and approximately three-quarters (76.0%) had a bone deformity.
Table 3 presents a comparison of CSHQ ratings between the patient group and the control group. When compared to the control group, the overall score (P=0.007) and the night waking (P=0.013), sleep duration (P=0.009), and sleep-disordered breathing (P=0.029) subscores were all substantially higher in the patient group. Although the patient group had greater levels of bedtime resistance (P=0.091), sleep start delay (P=0.547), sleep anxiety (P=0.105), daytime sleepiness (P=0.711), and parasomnias (P=0.200), these results did not reach statistical significance. Furthermore, higher scores were found for sleep disorders in SCD patients than in patients with thalassemia.
In order to address the research gap related to sleep disorders in children with transfusion-dependent hemoglobinopathies, the purpose of the present study was to compare sleep problems between children with transfusion-dependent hemoglobinopathies and healthy controls. According to the comments of the children's parents on the CSHQ scale, the researchers in this study compared the sleeping patterns and behaviors between these two groups of children.
Several reports have described difficulties sleeping among children and adolescents who have hemoglobinopathies. The majority of these findings are linked to SCD, a hereditary hemoglobinopathy that is characterized by persistent hemolysis and increased extramedullary hematopoiesis similar to that seen in thalassemia. However, relatively little research has investigated the connection between thalassemia and sleep disorders [37].
We identified evidence of disturbed sleep in a clinical sample of children with transfusion-dependent hemoglobinopathies. By all measures, the sleep disturbances in our sample, compared to published samples of healthy children, were severe, in agreement with the findings of other studies. In a study conducted by Tarasiuk et al. [38], the authors concluded that children and adolescents with beta-thalassemia or congenital dyserythropoietic anemia type 1 showed impaired sleep function, which was partially related to periodic limb movements and arousals that result in daytime sleepiness. Another study designed by Sritippayawan et al. [39] showed higher prevalence rates of OSA in children with severe beta-thalassemia. Our findings in this study were consistent with the literature. Parents of children with beta-thalassemia major reported more sleep disturbances than those of healthy children. Furthermore, night waking and sleep-disordered breathing were reported to be more common in children with beta-thalassemia major. Reporting these two types of sleep problems together may be an important point, since it may be speculated that sleep-disordered breathing could cause children to wake up more often during the sleep period.
There is a lack of understanding of the mechanism behind sleep disorders in children with beta-thalassemia. Kapelushnik et al. [40] described a child with both OSA and thalassemia intermedia. They hypothesized that the child's OSA was caused by extramedullary hematopoiesis in the nasopharyngeal region. All of the patients in the study by Sritippayawan et al. [39] who had OSA also had adenoid hypertrophy, and 80% of them also had related tonsil enlargement. All of the lymphoid tissues found in the adenotonsillar region had reactive lymphoid hyperplasia in their investigation, but there was no indication of extramedullary erythropoiesis. The authors hypothesized that lymphoid hyperplasia could be connected to recurrent infections of the adenotonsillar tissue, similar to SCD [41].
The limitations of the current study should be taken into consideration when judging the significance of its findings. The fact that we relied on information from the parents is a significant constraint [41,42]. Their interpretation of the child's condition can be colored by the difficulties they are experiencing as parents. For instance, depressed parents may have a more pessimistic outlook on their childrenŌĆÖs quality of sleep [43]. Both polysomnography and actigraphy are objective measurements that may be used to precisely assess whether or not a child or teenager is experiencing sleep issues [43,44]. Another disadvantage is that no family or environmental factors were considered, such as marital issues, socioeconomic position, or the setting in which the subject slept. There is a possibility that these factors can also affect young childrenŌĆÖs sleep quality [41].
In conclusion, transfusion-dependent hemoglobinopathies may increase the risk of sleep disturbances in children and adolescents, particularly those with SCD rather than thalassemia. Hence, assessing children with transfusion-dependent hemoglobinopathies during their routine clinical check-ups is crucial. Disrupted sleep has been linked to poor cognitive and scholastic performance, behavioral difficulties, and symptoms of depression and anxiety [19-21]. Sleep issues may make it harder for children to function, develop, and manage the main symptoms of beta-thalassemia. For patients with this disease, regular clinical evaluations should examine sleep disorders, including insomnia, nocturnal awakening, sleepwalking, sleep apnea, and daytime sleepiness. Managing children's sleep concerns may also improve therapeutic compliance. Working with parents to improve the sleeping environment may improve sleep quality and quantity (for example, by making the surroundings calmer). Educating parents and children on efficient sleep and bedtime routines at regular healthcare visits may improve children's sleep efficacy.
Notes
Author contribution
Conceptualization: MAE. Data curation: MAE. Formal analysis: AMA. Methodology: AMA and ADM. Project administration: AMA. Visualization: ADM. Writing-original draft: AMA. Writing-review & editing: ADM and MAE.
Table┬Ā1.
Distribution of children according to their sociodemographic and clinical characteristics
Table┬Ā2.
Distribution of clinical characteristics in the patient group
Table┬Ā3.
The comparison of CSHQ scores between the patient and control groups
References
1. Khandros E, Kwiatkowski JL. Hemoglobinopathies. In: Fish JD, Lipton JM, Lanzkowsky Pet al. editors. Lanzkowsky's manual of pediatric hematology and oncology. 7th ed. London: Academic Press; 2022. p. 161-92.
2. Makkawi M, Alasmari S, Hawan AA, Shahrani MM, Dera AA. Hemoglobinopathies: an update on the prevalence trends in Southern Saudi Arabia. Saudi Med J 2021;42:784-9.



3. Arpaci A, Elmacioglu S, Unlu B. Hemoglobinopathies. Int J Med Biochem 2019;2(Suppl 1):26.
4. Peslak S, Sayani F. Hemoglobinopathies and thalassemias. In: Pyeritz RE, Korf BR, Grody WWet al. editors. Emery and Rimoin's principles and practice of medical genetics and genomics. 7th ed. London: Academic Press; 2023. p. 143-72.
7. Sundd P, Gladwin MT, Novelli EM. Pathophysiology of sickle cell disease. Annu Rev Pathol 2019;14:263-92.



8. Kanter J, Liem RI, Bernaudin F, Bolanos-Meade J, Fitzhugh CD, Hankins JS, et al. American Society of Hematology 2021 guidelines for sickle cell disease: stem cell transplantation. Blood Adv 2021;5:3668-89.




9. Pinto VM, Balocco M, Quintino S, Forni GL. Sickle cell disease: a review for the internist. Intern Emerg Med 2019;14:1051-64.



10. Houwing ME, de Pagter PJ, van Beers EJ, Biemond BJ, Rettenbacher E, Rijneveld AW, et al. Sickle cell disease: clinical presentation and management of a global health challenge. Blood Rev 2019;37:100580.


11. Baird DC, Batten SH, Sparks SK. Alpha- and beta-thalassemia: rapid evidence review. Am Fam Physician 2022;105:272-80.

12. Hassan T, Zakaria M. Updates in thalassemia. In: Zakaria M, Hassan Tet al. editors. Beta thalassemia. London: IntechOpen; 2020 [cited 2023 Mar 27]. Available from: https://www.intechopen.com/chapters/72190
13. Ali S, Mumtaz S, Shakir HA, Khan M, Tahir HM, Mumtaz S, et al. Current status of beta-thalassemia and its treatment strategies. Mol Genet Genomic Med 2021;9:e1788.




14. Guilliams KP, Fields ME, Dowling MM. Advances in understanding ischemic stroke physiology and the impact of vasculopathy in children with sickle cell disease. Stroke 2019;50:266-73.



15. Abulhamail A, Selati S, Alasqah R. The association between obstructive sleep apnea and stroke in sickle-cell disease children. Eur Arch Otorhinolaryngol 2022;279:843-51.



16. Gillespie ML, Spring MR, Cohen RT, Klings ES. The interplay of sleep disordered breathing, nocturnal hypoxemia, and endothelial dysfunction in sickle cell disease. Prog Pediatr Cardiol 2022;68:101602.

17. Gileles-Hillel A. Sleep in sickle cell disease. In: Gozal D, Kheirandish-Gozal Let al. editors. Pediatric sleep medicine: mechanisms and comprehensive guide to clinical evaluation and management. Cham: Springer; 2021. p. 581-93.

18. Gois CR, DŌĆÖAvila J, Cipolotti R, Guimaraes L, Neto JS, Oliveira H. Association between adenotonsillar hypertrophy and sickle cell disease in adolescents. Pediatr Pol 2019;94:347-50.
19. Raghunathan VM, Whitesell PL, Lim SH. Sleep-disordered breathing in patients with sickle cell disease. Ann Hematol 2018;97:755-62.



20. Bouya S, Hashemi SM, Hormozi M, Moulae N, Mohammadi M, Imami A. Comparison of sleep disturbance among patients with cancer and thalassaemia and healthy controls: a cross-sectional study. Medycyna Paliatywna 2021;13:93-6.

21. Meltzer LJ, Williamson AA, Mindell JA. Pediatric sleep health: it matters, and so does how we define it. Sleep Med Rev 2021;57:101425.



22. Williamson AA, Mindell JA, Hiscock H, Quach J. Child sleep behaviors and sleep problems from infancy to school-age. Sleep Med 2019;63:5-8.



23. Stores G. Aspects of sleep disorders in children and adolescents. Dialogues Clin Neurosci 2009;11:81-90.



24. Lunsford-Avery JR, Baroni A. Pediatric sleep disorders: a unique opportunity for child and adolescent psychiatry. Child Adolesc Psychiatr Clin N Am 2021;30:xv-xvii.


26. Ramar K, Malhotra RK, Carden KA, Martin JL, Abbasi-Feinberg F, Aurora RN, et al. Sleep is essential to health: an American Academy of Sleep Medicine position statement. J Clin Sleep Med 2021;17:2115-9.



27. Singh J, Yeoh E, Castro C, Uy C, Waters K. Polysomnography in infants with clinical suspicion of sleep-related breathing disorders. J Clin Sleep Med 2022;18:2803-12.



28. Isaiah A, Pereira KD, Das G. Polysomnography and treatment-related outcomes of childhood sleep apnea. Pediatrics 2019;144:e20191097.


29. Jiang W, Bhattacharjee R, Nation J, Brigger MT. Completion of postoperative polysomnography for children with severe obstructive sleep apnea: a quality improvement project. Laryngoscope Investig Otolaryngol 2022;7:1667-74.




30. Bae E, Kwak N, Choi SM, Lee J, Park YS, Lee CH, et al. Mortality prediction in chronic obstructive pulmonary disease and obstructive sleep apnea. Sleep Med 2021;87:143-50.


31. Małolepsza A, Kudrycka A, Karwowska U, Hoshino T, Wibowo E, Pal Bojti P, et al. The role of screening questionnaires in the assessment of risk and severity of obstructive sleep apnea: polysomnography versus polygraphy. Adv Respir Med 2021;89:188-96.


32. AlNabhani A, Shapiro CM. Survey tools and screening questionnaires to pediatric sleep medicine. In: Gozal D, Kheirandish-Gozal Let al. editors. Pediatric sleep medicine: mechanisms and comprehensive guide to clinical evaluation and management. Cham: Springer; 2021. p. 135-58.
33. Spruyt K. A review of developmental consequences of poor sleep in childhood. Sleep Med 2019;60:3-12.


34. Hauri PJ. Sleep disorders. In: Gatchel RJ, Baum A, Singer JEet al. editors. Handbook of psychology and health. London: Routledge; 2021. p. 211-60.
35. Owens JA, Spirito A, McGuinn M. The Children's Sleep Habits Questionnaire (CSHQ): psychometric properties of a survey instrument for school-aged children. Sleep 2000;23:1043-51.


36. Asaad T, Kahla O. The ChildrenŌĆÖs Sleep Habits Questionnaire: psychometric sleep assessment instruments (Arabic version). Cairo: Nahda Press; 2001. p. 11-3.
37. Gileles-Hillel A, Kheirandish-Gozal L, Gozal D. Hemoglobinopathies and sleep: the road less traveled. Sleep Med Rev 2015;24:57-70.


38. Tarasiuk A, Abdul-Hai A, Moser A, Freidman B, Tal A, Kapelushnik J. Sleep disruption and objective sleepiness in children with beta-thalassemia and congenital dyserythropoietic anemia. Arch Pediatr Adolesc Med 2003;157:463-8.


39. Sritippayawan S, Norasetthekul S, Nuchprayoon I, Deerojanawong J, Desudchit T, Prapphal N. Obstructive sleep apnea among children with severe beta-thalassemia. Southeast Asian J Trop Med Public Health 2012;43:152-9.

40. Kapelushnik J, Shalev H, Schulman H, Moser A, Tamary H. Upper airway obstruction-related sleep apnea in a child with thalassemia intermedia. J Pediatr Hematol Oncol 2001;23:525-6.


41. Daniel LC, Grant M, Kothare SV, Dampier C, Barakat LP. Sleep patterns in pediatric sickle cell disease. Pediatr Blood Cancer 2010;55:501-7.



42. Graves JK, Jacob E. Pain, coping, and sleep in children and adolescents with sickle cell disease. J Child Adolesc Psychiatr Nurs 2014;27:109-20.




- TOOLS
-
METRICS

-
- 0 Crossref
- Scopus
- 2,061 View
- 49 Download
- Related articles in Ann Child Neurol
-
Assessment of Parenting Attitudes by Children and Adolescents with Migraine2022 October;30(4)
A Study of Epileptiform Discharges in Children with Chronic Recurrent Headaches.2006 May;14(1)